
Nearly 1 million total knee replacement procedures are performed in the U.S. each year and that number is expected to continue rising exponentially to over 3 million in the next 15 years!
So it comes as no surprise that the most common joint replacement procedure Physical Therapists rehab in the outpatient clinic is a total knee arthroplasty or total knee replacement.
Table of Contents
- What to expect after knee replacement surgery
- How long does it take to recover?
- Recovery at Home and Outpatient therapy
- Knee Replacement Exercises and stretches
- Walking After Knee Surgery
- Alternatives to Knee Surgery
- Life after a Total Knee Replacement
Many candidates want to know what to expect after a total knee replacement before they choose to have the surgery. Patients usually elect to have this procedure after nonoperative treatment options or knee replacement alternative surgeries fail to maintain knee function and pain levels.
For those patients that do decide to have total knee surgery, keep reading to learn more about the total knee replacement recovery process.
Read My Book on Total Knee Replacements Here!
- Fraticelli, DPT, Tim (Author)
- English (Publication Language)
What to Expect After Knee Replacement Surgery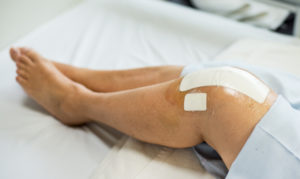
Typically a patient’s knee will be swollen, stiff, weak, and sore following surgery. This makes functional activities such as walking and standing up difficult to perform.
The timeline for regaining strength and range of motion after knee replacement is variable. These two elements are key to successfully completing the total knee replacement recovery process.
How Long Does it Take to Recover From Knee Surgery?
The timeline for recovering varies from patient to patient, but typically the rehabilitation process takes 10-12 weeks of therapy to reach goals of achieving range of motion, strength, and performing functional activities such as standing from sitting, walking, and climbing up/down stairs independently – without difficulty or pain.
Hospital Stay
The start of rehabilitation begins in the hospital soon after surgery. Pain levels, range of motion, and strength will be monitored to ensure progress is being made.
Patients will be assessed on day 1 or 2 to determine how much assistance is required with:
- Moving in and out of a bed to a chair
- Walking (likely with a walker or cane)
- Going up/down stairs
- Transferring in/out of a vehicle – since you’re not walking home!
Discharging home depends on the status of a patient’s knee healing, flexibility, and strength.
Patients are often provided with basic, but important beginner exercises to perform while in bed for regaining the necessary straightening (extension) and bending (flexion) of the knee, as well as early mobility to prevent blood clots.
Patients and family will also be educated on managing swelling, pain, and monitoring the incision site for bleeding, blood clots, or infection.
Blood clots can cause lower leg pain at rest in the calf area that is unrelated to the incision site itself and can cause increased swelling below the knee that is painful in the calf, ankle, and foot. Sitting still after surgery can create an environment for blood clots, so performing exercises while sitting or lying down is better than nothing.
Signs of infection include severe pain with or without activity and abnormal redness, tenderness and increased drainage at the incision sight.
How Long Will I Be in the Hospital After Total Knee Replacement?
The length of hospital stay after knee replacement will depend on:
- Replacement and incision healing routinely.
- Manageable pain levels.
- The patient being able to perform bed mobility and walking without requiring someone else doing the majority of the work for them
- Help at home from family or friends for activities that will require assistance such as driving, cooking, cleaning, moving in and out of bed, sitting down and standing up, walking, or using stairs
These are important for ensuring a patient is safe to go home. The majority of patients meet these requirements and will be out of the hospital within 1-3 days.
If a patient has delayed healing or limited support at home, they may be a candidate to be transferred to a skilled nursing facility or rehabilitation hospital for 1-2 weeks for further recovery.
Knee Replacement Recovery at Home and Outpatient therapy
It would be nice if a knee replacement was like getting a new car part installed and away you go. The surgery is just the beginning of the knee rehabilitation process.
Swelling, stiffness, and strength are necessary to improve in order to decrease pain and progress therapy to higher level activities. They will be the primary focus of therapy early on to set up the patient for successful rehabilitation. It will take time for the knee tissues to heal and gradual loading to improve strength and flexibility.
Swelling After Knee Replacement
Leg swelling is going to be present after having a knee replaced. Swelling has a significant effect on knee flexibility and the ability for muscles to contract. Think of trying to roll up a full water hose versus an empty water hose.
It is important to monitor, limit, and attempt to reduce swelling as much as possible.
Swelling management strategies include:
-
- Laying down with the surgical leg straight and elevated above the level of the heart with an ice pack for 20 minutes of every hour.
- A compression and cold therapy unit such as GameReady, Squid Compression, or Cryocuff may help to limit and reduce swelling.
- Laying down with the surgical leg straight and elevated above the level of the heart with an ice pack for 20 minutes of every hour.
- Performing ankle pumps, knee bending and straightening, and moving the hip in all directions every 20-30 minutes will prevent having too sedentary of an environment.
- Avoiding having knee in a gravity dependent position or below the level of the heart for too long (i.e. standing or sitting still for prolonged periods).
- Wearing appropriate fitting compression stockings or socks may aid in reducing swelling as well.
It is also important to continue monitoring for blood clots and infection, as sometimes the onset of symptoms is delayed and requires immediate medical attention, possibly rehospitalization.
Knee Replacement Range of Motion
Knee swelling will limit knee flexibility, but there is also healing and scarring of tissues to consider that will prevent a knee from bending and straightening. Patients need to slowly improve their flexibility so their knee does not heal stiff, but at the same time not push too much that they are aggravating the recovery and causing more swelling.
The “normal” knee range of motion is 0 degrees of knee extension (straight) to 135 degrees of knee flexion (fully bent). It is not unusual for someone to have 5-10 degrees of hyperextension and knee flexion varies anywhere from 120-150 degrees.
The expected range of motion after knee replacement is 0 degrees of knee extension to at least 115 degrees of flexion or greater, but this can take several weeks or months to achieve. Starting out, the goal is to get the knee to bend to 90 degrees within the first week and then improve 5 to 10 degrees each week after that until full flexion is reached. Again, this timeline is variable from patient to patient.
It is important to achieve full knee extension for walking to feel more natural and have less knee pain. If you don’t achieve full extension, it will feel like you’re walking with 1 leg shorter than the other.
Read My Book on Total Knee Replacements Here!
- Fraticelli, DPT, Tim (Author)
- English (Publication Language)
Knee Replacement Exercises
Strengthening after a knee replacement is just as important as managing swelling and regaining knee range of motion.
After surgery, a physical therapist will guide each patient through total knee replacement exercises. Having a PT provide guidance will be helpful as it can be difficult to engage the muscles of the leg in order to achieve the motion into flexion and extension. As mentioned above, the motion of extension (straightening the knee) and flexion (bending the knee) will be a focus early on with the rehab process. Below is an outline of the exercises you can expect to perform during Physical Therapy.
Knee Extension Stretches and Exercises
Expect to perform a variation of these knee extension exercises:
- Quad Sets
- Straight Leg Raises
- Short Arc Quads
- Long Arc Quads
- Glute Sets
- Supine foot prop
- Seated foot prop
- Passive Range of Motion
- Overpressure
- Contract/relax
- Seated calf stretch with towel/belt
- Standing TKE
- Prone TKE
- Knee Flexion Stretches and Exercises
Knee Flexion Stretches and Exercises
It is vital to achieve full knee flexion to:
- Sit without having surgical leg sticking out (think sitting in a car or airplane)
- Bend knee to go up and down stairs or an inclined walkway
- Make dressing easier (think putting socks and shoes on)
- Ride a stationary or road bicycle
Expect to perform a variation of these knee flexion exercises:
- Ankle Pumps
- Heel slides
- Supine
- On wall
- Seated
- Partial Squats to chair
- Seated Knee Bends
- Quad stretch
- Sidelying
- Prone
Some patients will use a continuous passive movement (CPM) machine that will repeatedly assist bending and straightening your knee slowly for hours each day for a couple weeks until they have reached a desired range of motion.
Walking After Knee Surgery
As previously mentioned, walking after knee surgery will likely begin the day of or day after surgery in the hospital with a walker or cane. The amount of weight put on the surgical leg is usually as much as tolerated, so using the walker and taking smaller steps can help offload a painful knee. The goal of walking early is to prevent muscles from weakening and to get the knee moving in a normal gait pattern again.
Patients that are hesitant to walk or use the walker as a “crutch” for too long can also delay the recovery process. This goes back to the “as tolerated” concept. If you can tolerate walking without a walker, then walking starts with short bouts until longer distances are comfortable.
When Can I Stop Using a Cane after Knee Replacement?
Within two weeks of surgery, some patients may walk without any device in the morning, but become tired in the afternoon and need the device again. The same concept applies to changing surfaces (carpet, tile, grass, pavement), inclines, or steps. It may be easier to walk in the house on a firm and predictable surface without a cane or walker, but going outside on uneven and unpredictable ground would be safer with an assistive device.
On the other hand, walking without a limp while using a walker will be necessary before moving on to walking with a cane or no assistive device at all. Tossing the walker or cane to the closet too soon can cause delayed recovery and possibly not regain a normal gait pattern.
Almost every PT has had a “strong-opinionated” patient that chose to walk without a walker or cane before the therapist was in agreement and had less successful outcomes in terms of their walking abilities. It is highly recommended that an assistive device is used for as long as needed to achieve the required strength, flexibility, and gait pattern.
This process requires patience and understanding from the patient that every surgery and recovery is different. This means that even though someone they know was walking without a walker after surgery before they are that they are not necessarily behind.
Alternatives to Total Knee Replacement Surgery
There are several different conservative or less invasive options that may be attempted prior to having a total knee replacement.
Injections are often used in an attempt to decrease inflammation, friction, and pain in the joint. Surgical options to consider aim to preserve or restructure remaining tissue and to prevent or put off a total knee replacement.
Physical Therapists provide non-invasive treatment options to improve strength, flexibility, and body mechanics for functional activities to reduce knee pain. PTs can also educate patients on an exercise program for improving body composition.
Life After Knee Surgery
As a Physical Therapist, I’ve seen firsthand the significant improvements in people following a knee replacement. However, there is no surgeon or PT out there who can 100% guarantee success. There certainly are risks following a surgery and this should be discussed with your doctor. But just as important, you should discuss the expected outcomes with your physician.
Returning to activities such as walking, golf, bowling, swimming, light dancing, and even light tennis is usually encouraged. However, ask your doctor about suggested timeframes for these activities.
Knee replacements have come a long way in the past 20 years and the technology continues to improve. Set your expectations appropriately with your physician and therapist. Here’s to hoping your life after knee surgery is full of enjoyment and activity!
Read My Book on Total Knee Replacements Here!
- Fraticelli, DPT, Tim (Author)
- English (Publication Language)



My dad has to get knee surgery soon, and he is wondering what to expect after surgery. That is good to know that the timeline for regaining strength and range of motion will be different for everyone, but usually takes around 10-12 weeks. That isn’t too long. I think my dad will be fine. Thank you for all the information about what will happen after his surgery.
Glad you found the article to be helpful!
Let your dad know it’s painful after surgery! Everyone told me you’ll love your new knee…NO ONE said there is pain for the first month! The physical therapy is no joke!! It’s a lot of work, and very important to get your extension and flexion to the best possible range. I wish I would have known this.
Every time I stand or walk while working I find it hard to get out of my car and my knees seems to be very heavy when I get home. I am at ten weeks post surgery I am afraid I have blood clots. Is this pain normal?
11 weeks post op. My knees feel very heavy. How long does this last? I had both knees done at the same time. No pain at all they just feel heavy.
I am very glad you had no pain and would like to know how. MINE WAS AND is still painful.
June 4th will be 4 weeks from TKR – doing outpatient PT now – I’ve been walking without aid of cane/walker 10 days after TKR – ROM is slowly getting there – overall I’m very pleased. I’m a 5’11 190lb 75yr old former runner (42 yrs).
Great to hear Gary! I hope you’re feeling great now!
I am progressing after tkr
The biggest thing I found was that you have to control the pain so you can do the exercises. If you don’t then you won’t put the effort needed to exercise and then that’s when problems happen.
I’m walking fine just at eight weeks.
Do the exercises.
I will be have. Knee surgery soon.Thank for the information.
Good Luck! Work hard and you’ll do great!
Going for tkr in a few days. This article has been very helpful to put concerns aside. Thank you.
Good Luck Marie!! Glad you found the article to be helpful 🙂
I had my total.on Feb. ,26 2018. A two day stay in the hospital. Before having my tkr I did many exercises which were in the booklet the hospital provided. It is very important to do these exercises to build your leg muscles b4 your surgery. Follow your doctor’s recommendation and do your exercises from phase ,1. After a month you will see a physiotherapists follow all their instructions. I am not saying it is a easy process as you will have pain and tightness in the back of your calf. You will having bruises on the heal of your foot and on your thigh and leg. Your leg will feel tender to touch. Do not be alarmed this is all normal. Do not forget you need to elevate your leg daily at least 5x a day plus icing you knee. Also do not push yourself to the extent of not using the Walker at least for two wks than the two crutches. The final phase down to one crutches. If you go faster then that it could slow down your recovery. As each person heal at their own rate keep in mind 100% recovery could take a full year. You are learning to walk with replacement parts and it takes time. In 10 days I start my physiotherapy
Great insight Susan! It’s true, everyone’s recovery is different and you’ve shared some great insights on your journey so far. Thanks for taking the time to read the article and to share your story!
I had TKR 8 months ago and I still use my walker and I am 75 years old. Three years prior to my surgery I had a ICH stroke and it affected my right side. I have been using a walker since the stroke. I do all my exercises but am disappointed that I am not healing as fast as I think I should. I was very active before the stroke. One person told me it would take a good year. Is this normal? Thanks for any insight you can give me
Hi Earline,
Thanks for commenting and sharing your situation. What were your expectations for the surgery? If you had been using a walker for the past 3 years due to the stroke, a total knee replacement isn’t going to change the residual effects of a stroke.
In general, a knee will continue to change for an entire year following a TKR. The swelling can continue to fluctuate for an entire year.
Tim
Had a TKR On 3/6/18 (right knee) and am doing very well. Walk with a cane outside. PT 3x a week and am up to 103 degrees of flexion. However, this is the antithesis of what happened last year with my left knee. Horrible swelling and pain. Took 13 weeks to recover well enough to return to work. I believe the reason to be that I waited too long bf I had the surgery. My left knee was in terrible shape by the time I had surgery. I decided to do the right one now bc it was in better shape and as I’ve been told numerous times, “no two knees are alike”. Luckily, that is true in my case. My recovery is surprising but certainly welcomed after my history. Hard work, diligent exercises and time are the keys. I wish all here the very best.
I had a knee replacement on Oct 12, 2017. I was walking on uneven ground and afterwards have a searing pain on the side of my knee. It still hurts after two days. Should I only be walking on paved surfaces from now on?
I didn’t know that bumpy ground would cause knee pain. Thanks.
That’s a good question Addie. Walking on uneven surfaces is no doubt more difficult due to the challenge of balance and instability many people have after a total joint replacement. The good news is that balance and stability can be improved with practice, so a gradual re-introduction to this type of activity may be beneficial.
Walking on a paved surface may be the best option for people who have just had a total joint replacement. Progressing into a more challenging terrain is possible, but should be done gradually.
– Tim
Encouraged to finally read a comment about the condition of the joint before surgery. I had my TKR almost 9 weeks ago and have been very dilligent about exercise, icing, Rx, etc., yet it has been a real struggle for every degree of ROM. Specifically, I have just reached 110 flexion (gaining about 5*/week) and seem to be stuck at 5* extension. Very frustrating, to say the least! Especially when I see others at the physio clinic doing so much better (and so much sooner)!
I am 65, have a BMI under 26, spent 12 months of ‘prehab’ before the surgery and underwent a hip replacement (same side) 15 months before the TKR. HOWEVER, I ruptured my PCL 25 years ago, and was diagnosed with osteoarthritis more than 15 years ago. For a variety of reasons, I waited so long for this TKR that the knee and its surrounding structures were in horrible condition for many years BEFORE the surgery.
Nobody ever suggested that I should be prepared for a slower and, therefore, longer recovery due to my condition before the surgery. I think practitioners would be wise to warn patients that not only will rehab be a demanding and painful process, but it might well be slower if one has lived with knee disfunction for many years prior to replacement.
My aim is for a minimum ROM of 125 by 6 months and I will keep working to get there and stay active to keep it.
June 23 2018
I had a tkr on May 22 2018 I was delayed getting physio for 2 weeks due to medical issues. Now I am in rehab. I still have some swelling and bruising in the knee and struggling to get range of motion. I left hospital after 2 days and had a 80 degree bend. Little physio in hospital and surgeon had told me before surgery he expected his patients to have a 90 degree bend so this was not a good start for me as I was feeling a bit disappointed. My surgeon had said their would be a lot of pain but I was not expecting so much swelling and bruising in my thigh, knee, ankle and down the side of my leg. It does take patience a lot of patience and physio in clinic and at home.
Hi Patricia,
I hope you’re feeling better since your TKA. It is common to have bruising as you’ve described. The swelling can really make it difficult to achieve a 90 degree ‘bend’ or flexion of your knee.
I’d be interested to hear how you are doing now. Hope you are well.
All the best,
Tim
This operation is a breeze compared to what I went through with the same knee 30 to 40 years ago I’ve never been so good Barbara swanson
Hello Alleson,
Thanks for sharing this (aware of date). I’m in this position now. Yes it’s only been 2 wks OP. But I’m concerned of the lack or minimum ROM. I was informed that during surgery it was discovered that my knee was worst than the X-rays showed thus making me wish that I had had TKRS before now. I’m 52 years young 😜 and wish to have a better quality of life with my knees and life un general. There was a period of time I experienced pain and discomfort etc on a daily basis for many years. I have had several courses of PRR, nerve ablations and steroid shots and while there was some relief, my fall on both knees (they gave way) earlier this year, on tiled floor was the deciding factor of either now having continuous steroid shots (my last option b4 TKR) when to have TKRS.
As I do live alone, I decided “its time!”
I imagined it was as with any or parts else of the body, time heals all wounds. Looking forward to improved ROM, minimal since po. Thank you for the information to gain better understanding of these changes my body is going through and what possible expectations are.
Wishing you and everyone else speedy and complete recovery 🙏🏾
For those of you considering a bilateral total knee replacement here are some observations I have made at day 6 of recovery. You need to be in good physical shape before attempting it, expect what I was told and have experienced – greater total pain, less mobility at first since you don’t have a “good leg” to help you, and a post operative feeling of “what the heck what I was thinking?” when I asked for a bilateral. Days 1-4 1/2 were real rough. Day 4 1/2 became more tolerable and now in day 6 I see hope! There was too much pain for the first three days for barely any mobility exercises but am into them now and have about 80 degree ROM. I look upon my recovery program as my job and have no illusions about the tough road ahead. At this point I think that really the main difference between one knee or both knee replacements is the increased demands placed upon your caregiver for a bilateral for reasons stated above. I also managed to somehow come home with a UTI which I have never had before. Actually there is one advantage of having a UTI at this stage – I have no choice but to frequently get up and using the walker, go the bathroom thus exercising the knees rather than staying too long in bed or the recliner before getting up. Hope these observations help those of you contemplating a bilateral.
I am very heavy, and both of my knees are really bad (down to bone-on-bone on the insides and behind the knee caps). My surgery for my first knee is in 2 1/2 months. I am worried about recovery and PT with the other knee being in such bad shape. Also, after reading this article and the comments of others, I am worried that I will be able to schedule my second knee three months after the first. Any advice? (I’m trying to lose weight.)
Karen I hope you only listen to your doctor. If the doctor said to lose weight, I hope you do what he says. Because when a person has extra pounds on their body it is not good for your knees. The legs and knees over the years has to hold up more weight and they
will tire out and over the years wear out.
Hi Karen – hope you get this message. I’m also quite overweight, and had a TKR eight weeks ago. I’ve had an exceptionally good recovery, which I attribute to my surgeon’s skill, my exceptionally strong leg muscles, a high pain threshold, and a fair bit of determination. I would say the best thing you can do at this point is to work really hard on strengthening your quads & hamstrings, since they will be important in supporting the new knee, and your entire body, after surgery. If you can get to a gym, you’ll be able to get specific information on strengthening those muscles. My other knee will be done approx. 6 months after the first one, which seems a reasonable period of time for the first knee to be fully stable and able to support me while the second knee recovers. Try not to be afraid – this is a really positive thing that you are doing for yourself, and once you are pain-free and mobile, you’ll be better able to deal with weight loss issues. Best of luck to you!!!
I am also heavy, but I exercised with heavy weights and did cardio 4-5 days a week 1.5 years before surgery and got more heavy tho to muscles. I had total kneereplacement in both knees at the same time. My surgeon meant that i was physical and mentally strong enough to handle it. Day 8 i went back to the gym and in week 12 i went hiking twice in 5 days . My bend was at 135 week 8 and i been doing my exercise 4 times a day until week 12. I had no fysioterapi and i’ve been taking care of all the rehabilitation on my own. Today it’s 5 month ago and i’m doing fine. Still in pain and stiff but hey, i can walk again and go hiking. Hiking is my passion in life and i love it! And i’m only 44 years old and i have had problems with my right knee since i was an elite swimmer at the age of 16 and I’ve been doing kickboxing for many years in until the age of 32. That’s when my knee got realy bad. Unfortunately my left knee ended up being the worst knee 🙁 But here i am doing what i love the most thanks to two new knees!
I am at odds with the physio who is measuring my knee flexion post KRS. She insists that I am sitting on a chair with my whole foot on the floor and that I slide that back towards me. When I cannot do so without lifting my heel off the floor that is my maximum knee flexion.
I used to be a rehab PT and my understanding is that you do not measure flexion of a joint when evolving TWO joints (in this case the flexion of the knee and dorsi-flexion at the ankle).
For example if my ankle was injured and locked at 90deg to the tibia, because I could not lift my heel off the ground it would appear that my knee would have very little flexion at all!
I would be interested in your comments.
After discussions with the surgeons and the senior physiotherapists they have confirmed that the methodology used as I reported was incorrectly applied.
The individuals involved had mistakenly used a measure for early post-operational flexion (when flexion is extremely limited) and applied it to later stages in the treatment cycle when there was, in fact, much more flexion.
The result of this was that the degree of knee flexion was under-reported, giving the impression that recovery was slower and extended physio treatment. This has now been corrected.
I had TKR on both knees in Jan 2018. When I walk, exercise or stand up
I feel the knee replacement moving. Is that normal
It’s common to feel the prosthesis (the new knee) move a little or make small clicking noises. Nearly every TKA I feel will have a small amount of give to it that may feel like it’s ‘moving’ as you’ve described. As your muscles become stronger, the knee should feel more stable with those activities.
Had total knee replacement 6 weeks ago and I can say I am now feeling better. I am 71 and I also am heavy. The first 2 weeks are the hardest with pain but from word go I did very good with walking. I will say I don’t like pain meds so I think I had more pain because I would only take meds when needed and I was wrong about that..I only had 4 weeks of therapy and was released with ROM at 110. I do the therapy at home 2 times a day and I don’t fudge on this..i am religious about that…I had trouble sleeping for the first 3 weeks but that also is getting better. When back to work in 3 weeks no drove car in 2 weeks. So all in all I am glad I had it done so far…I need the other one done also but I will wait for about 6 months..
Thanks for sharing your experience here Cathy! Glad to hear that you’re doing well. All the best!
-Tim
yes my doctor say that recover within 8-10 months but i need more time above 1 years don’t know why, i think for my eating habit. and for that still now i fell some pain when i walk so much. i take continue medicine from my doctor prescription. hope it will be fine within months.
but thanks for sharing your great article.
Great insight Susan! It’s true, everyone’s recovery is different and you’ve shared some great insights on your journey so far. Thanks for taking the time to read the article and to share your story!
Hi All,
I had TKR on my right knee on September 24th which was about 10 days ago. I had the left done about 8 years ago so I knew what I was in for as far as recovery; then it was about 6 months for me to have no lingering discomfort.
For this procedure (now at 10 days), I’ve had a PT evaluations and two sessions. Needless to say, the sessions were heavy duty and I was pretty exhausted at the end. After the second session which went well, I suddenly had a break through and was not as sore. The calf muscles and tendons seem to be taking the brunt of the load but with ice and a lot of at-home follow-up stretching and am moving along and looking forward to getting a few days of rest (I’ll still work at home on key exercises). I am pretty well over needing the walker but will not switch to a cane until instructed.
One thing I had not counted on was the fatigue. It seems that 4 hours of activity in the Am and it is time for a nap. Then some afternoon activities and a nap before dinner. Are other experiencing this?
I do ice several times a day, wear my compression sock, and find myself unconsciously doing leg and knee stretches and I watch TV. There seems to be a decrease in swelling but the fatigue was a surprise.
Is it just my body say “take a rest…”
Hank
PS I’m just about off all serious painkillers and just use acetaminophen as required.
I’ve had five knee replacements on right knee. I rode from Chicago to DC, my knee feels like post op surgery pain. It’s stiff and painful to stand. I got to ride back to Chicago on Sunday. Feedback greatly appreciated. Thank you in advance.
Thank you for sharing this article. Hope it might be much useful for us. keep on updating !!
Im having tnt on 15th all my pain is in back if knee banker cyst they say its because knee has bad arthritis bone spurs will cyste go away after New knee?
I’m having my right knee replaced on January 16th and I live a lone. I just moved to my new location and I don’t know anyone here. It’s scary and just wondering if anyone knows the time line to return to work if you walk all day and do have to do lifting?
Omg, I had the surgery on Dec 20th you are going to need someone at home to help you there is no way I could of made it without family!!!! I’m just starting to walk on a cane the experience hasn’t been good for me at all, I’m not sure when I’ll be able to return to work, I’m still in therapy at home right now two days a week, will see my surgeon for follow up again next month
Wanda can you tell what was so awful? Im a pretty tuff little cookie but I have to admit Im scared. Its been over a year for you. How are you doing?
Very thorough post, it points out every single point of knee replacement surgery recovery. Initially, i has several questions but now i am very crystal clear with every thing. Thank you writing this post.
I had tkr 9 weeks ago I am only taking ibuprofen for pain. I can be on my feet all day and do anything I want but I get tired. My problem is my range of motion is only 123. I had more prior to surgery. I still go to PT and exercise. Will I gain more or is this it?
I had TKR on 9 Jan this year. Since that time, I have a manipulation due to a stiff knee. I work hard at home on my exercises and never miss PT. Today, my flexion was 85. It keeps going up, but I guess it takes time and more time.
I agree with Teresa, everyone said it’s great, you’ll love it….but no one said how painful it was in the beginning. I had my TKR 7 weeks ago and I cannot imagine having the other knee done. Maybe later on I may but now the pain is still too fresh to consider it.
Thank you … I am four weeks post op and feel the same way you do.
I had TKR on March 5, 2019. I was released to go home on March 8, 2019. Home Health came on Sunday, and the workout was so rough that it took me until Tuesday to recover. Another PT came yesterday, and said my knee should bend 90 degrees by now, and pushed my leg back so far that my knee swelled and now I can hardly move it. I also have fibromyalgia, and osteoarthritis. Both hips have been replaced, and my other knee needs to be replaced. I’m 74, somewhat overweight, but was active before this surgery. Any advice? I’m discouraged!
I had bilateral tkr at the end of December (2018). For those concerned with pain, swelling, and rom, my advice is to do absolutely everything you can from minute 1 to gain as much extension AND flexion as possible. Move those knees. I gained 140 and 0 very early on. Ice as often as you need. There is so much soft tissue damage that it will take time for pain and swelling to go down. Look for small improvements each day. It does get better. I made daily notes about my sleep, medications, activity, and thoughts so that I could look back and see my progress.
Rt knee on 26/4/2018 and lt knee on 12/9/2018 with successful tkr at Kim’s sec,bad ts by Dr I’ve Reddy thanks now I walk with stick ocationally w/o but stiffness in mornings
I still have numbness and lack of strength on my left knee 19 months after robotic TKR. Should I go
on the ahead with surgery on my rt knee with this condition, or wait until the rt knee is in better shape?
Am 70 years old! Had TKR , Nov.26 2018 ! Need the other knee done but terrified with outpatient therapy! The therapist made me scream with pushing my knee down several times & pushing my knee against my butt several times! Was told outpatient therapy is painful & am not looking forward to a repeat performance!
I am 4 weeks post surgery and range of motion is 120 and 0. I had my knee replaced at an out patient facility and was home that night. I can now walk up stairs unassisted and very close to going down stairs without holding on. I am very diligent about doing my exercises daily in addition to PT now 2 x week. I feel like my gait for walking feels mostly normal. I do continue to have swelling towards the end of the day but always finish off the day with Ice. I also monitor the fullness feeling in my knee and is soon as I start to feel it I sit down and put my feet up. My PT says I’m about two weeks ahead of where I should be. I go for my six week check up in two weeks and hoping I might be cleared to golf. I think part of my success and recovery comes from all of the exercises I did prior to surgery. I was active and yoga, Pilates, and spinning/ cycling classes. My suggestion to anybody having total knee replacement would be to get your legs strong before the surgery and stay consistent after the surgery with the exercises they give you.
I have had a replacement in both knees in 2015. Due to aseptic loosening the right knee needed to be totally revised. I had that done September 10, 19. Today, three weeks post op, my Rom is a degree or 2 off of being totally straight to 110% bend. Weaning off of the cane this week and hoping to go back to tending bar a few hours a week in another month. I am 71 years old, 5’3 and 189 pounds. I believe I am doing remarkably well have been doing out of the home pt since 6 days post op. I did well all three times but kept moving before and after each surgery. Yes it will hurt, but use it! Good luck to everyone on your journey.
I have TKR on my right knee on June 3, 2019. I must say it is the best decision I have made and I should have done it sooner. The road was rather rough and it was painful and I did my physical therapy as recommended. In September 2020, I will be undergoing a TKR for the left knee.
Good to hear that you don’t regret it. I am starting with my right knee next month November 2020, and my doctor said his rule is, “as soon as I forget the pain from the first knee” it will be time to set up my left that is also 💯 bone on bone. I do t think I am comprehending the pain. I have had many surgeries, but they say this is totally different🥴 Hoping I have what it takes to make this a success.
I had a TKR mid August 2019, on August 2, 2019, my surgeon gave me an Iovera treatment, he injected a substance that froze three nerves above the knee and two nerves below, He deadened the area prior to the injections.
I needed No pain medication after discharge from the hospital, the day after surgery. I stopped using a walker 5 days post op, a cane 10 days post op and began driving two weeks after surgery.
Five months later the nerves have almost completely regenerated and still no pain.
Hello. I actually have a triple whammy going on. Both knees have had arthroscopic surgery, my right twice. Osteoarthritis in both knees. I also deal with neuropathy. When the knees get bad the neuropathy kicks in. Burning behind the knees, burning calves, burning feet. I am at the point where something needs to be done. Tired of being depressed. Seeing dr. next week to possibly schedule first knee replacement on my right. Very worried about how my left knee is going to handle it. Also, would anyone now how this surgery would affect my neuropathy? Any recommendations would be greatly appreciated. Thank you!
I am a right leg bk amputee done 10 yrs ago my left leg is my problem I know I need a knee replacement but don’t want to go to any rehab. how much problems will I have after I get this done but I am not able to sleep cause I am in so much pain. will I be able to do out pat. therapy. I am also 71 yrs old.
Margaret: I had tkr 17 days ago. I’m 76 and slightly overweight. For the first two days little pain and walking just small distance round the room. I Cannot put too much emphasis on using an ice pack. Five times a day for max 30 mins eases the discomfort greatly. Simple leg raising exercises, 5 raises to count of 6 x 5 a day. Self massage with Arnica oil or cream a few times a day. Knee bending 5 x 5 times a day. I’m a lazy woman so if I can do it, you can. Good luck. June 2020
I will be going in for my TKR in Nov 2020 on my Left Knee. I am 56 years old and active and work in Production so I am on my Feet daily and move around a lot. I live on my own and do live in an Upper Flat, so I am wondering about coming home from the Hospital or will they send me to a Rehab Center to stay for a week or two. I have had Surgery on this Knee before for Torn Menicusus and at that time the Surgeon cleaned out the Arthritis also. I had no issues with that Surgery and was able to recovery quickly and return to work within about 4 weeks. I do expect to be out for the full 3 months for the TKR. What do you suggest I get for at home to aid in my recovery in addition to my PT. As I will be trying to purchase most of what I need prior to my Surgery so that I have it at home for when I return.
I am having a TKR in November 2020 also. They told me to get a walker with front wheels and a cane. I opted for a quad cane for greater stability. I ordered several ice packs, As everyone says it really hurts,so I am hoping that with medication, elevating and ice packs it will be tolerable to be able to start physical therapy right away. I have 13 stairs to come up when I get home and they said it will be fine.
Hope everything goes well for you!!!
Had TKR in 2008 and it has been wonderful to be able to walk with out pain. Had no cartilage remaining in either knee and it was basically bone on bone. The at home Physical Therapist I had was a brutal little thing and I am thankful every day for her. The only problem I had was after a year I had a bad reaction in the left knee and had to have it replaced again. Believe me, the second time is not as much fun. But after 12 years, thanks to the medical staff and physical therapist, I am still at 90% original mobility and doing great.
My spouse is in the 7th week after Total Knee Replacement. He says he hopes he NEVER GOES THOUGH THIS AGAIN. He has more pain now ever since the operation. He does not like taking the pain pills, however, that is the only thing that gives some relief. This comes from a former disabled Marine! He has NEVER HAD PAIN LIKE THIS.
Oh know… Hope it better soon for him!!!! Did they use a nerve block during the surgery? My doctor said that it would really help the first couple days while I get the pain medication in me.
I am having a TKR in early November. I am bone on bone with both knees and if I try to walk the dog anymore I am up with Lyrica and Arthritis Tylenol and sometime Benadryl to help me get to sleep because both knees feel like someone took a sledgehammer to them. I also have a very weak feeling behind my knees. I have done over 3 years of injections to hold off as long as possible, but feel now I must have them done. My orthopedic surgeon says it is better to do one at a time, so I chose my right first and my left to follow ASAP. The only thing that scares me is that they are all saying it is extremely painful.I bought several ice bags and a walker to use as soon as I get home. It is a day surgery and I have 13 stairs when I get home. Am I wrong in thinking the pain medications and icing will make it tolerable?
The pain can be very extreme at least had a TKR done about 10 weeks ago and had severe swelling of leg/feet.I stayed in hospital two days then home im in PT now as outpatient but its tuff.
How did you reduce the swelling? I think the swelling is limiting my ROM now at 7 weeks post op.
I’m taking an nsaid, but it doesn’t take the swelling totally away.
Nancy
I had TKR in December 2020 I didn’t know it was so painful, and demanded so
much from a caregiver. For someone that never used strong pain killer
I was very careful I was afraid to get addicted. After 6 weeks I feel better but
still worry if i can have any complications from the surgery.
Can you make any recommendations for preparation for knee replacement?
My 87-year-old father has been referred for TKR. Probably 8 or 12 weeks will elapse before he actually has surgery. He has never been particularly compliant with Physical Therapy, and he has lost considerable muscle mass over the past year.
Are there specific exercises he could do preoperatively to improve the chances of a smoother, more successful recovery and perhaps a more satisfactory outcome?
Well written content like this restores my faith in quality writing. I finally found information I can agree on and use. Thank you for sharing.
I am so thankful to have found this site!! Excellent info! I am 7 days postop TKR for the right knee. Also right hip bursitis and 3 protruding discs lower lumbar, right side, of course! Getting that corrected next. My rom is 105 with -10 extension. No problem walking full weight. Still using walker but barely. My question is what the heck is normal rom and extension? Have had very little swelling. Pain has not been fun but a necessary evil and not the worst in the world. What should my goals be? Thanks so much for any help!!
i have a very physical job i do a lot of walking and heavy lifting i need a left knee replacement I’m concerned about if i can still do my job
This information was very helpful. My husband had tkr 12 days ago. We were given lots of information, but this article added to it and clarified some. For example, importance of elevating affected knee was mentioned, but this is first I’ve read that clarified leg should be above heart so we were not raising high enough. Also mentioning knee clicks and movement will abate as muscles build very reassuring. For those who gave not gone through this yet, I was recently told the first week is very tough (true); second week considerably better (also true) and third week better yet.
Also, nobody mentioned the extreme fatigue and stress to both patient and carer. We were told “Above all, you must not fall.” The stress worrying about that for the first week was crucial. Whatever prep of the environment you did pre-op, it will still be problematic, especially if the bathroom is not right there. Take your Doculax stool softener twice a day so you do not have to deal with constipation. Wear a pad or other undergarment because it is so hard to change the underwear and pj bottoms while you are standing in a walker, even with a grabber to help and a carer to help. We put a rug bedside and in front of La-Z-Boy and have a plastic pee jar ready because the first week or so you are often too slow to make it to bathroom so can just stand up in walker, take down pants and pee. Gross, but effective. Also, if you are a senior, you will have to pee several times at night when you and carer are half-asleep so that shortcut will help early on.
Have a pad and pen near meds and keep a log of meds to make sure you take the doculax, aspirin to prevent blood clots and to keep track of pain meds and Nsaids.
Thank you for this informative post! I recently underwent a total knee replacement, and your tips on recovery expectations have been incredibly helpful. I especially appreciate the section on managing pain and the importance of physical therapy. It’s reassuring to know what to expect during the recovery process.
Thank you for this informative post! It’s reassuring to know what to expect during the recovery process after a total knee replacement. I appreciate the tips and insights on managing pain and the importance of physical therapy. This has definitely eased some of my concerns as I prepare for my surgery.
Thank you for the detailed insights on knee replacement recovery! Your tips on managing pain and the importance of physical therapy are really helpful. I’m about to go through this surgery myself, and it’s encouraging to read about what to expect. Appreciate you sharing your experiences!
Thank you for sharing such insightful information about knee replacement recovery. I’m currently in the process of preparing for my surgery, and your tips on post-operative care and managing pain have been incredibly helpful. It’s reassuring to hear what to expect during recovery. Looking forward to following your advice as I embark on this journey!
Thank you for this informative post! I appreciate the detailed insights on what to expect during the recovery process after knee replacement. It’s comforting to know about the milestones and challenges ahead. Your tips on managing pain and the importance of physical therapy are particularly helpful. I’m feeling more prepared for my upcoming surgery!
Thank you for sharing such detailed insights on knee replacement recovery! It’s comforting to know what to expect during the healing process. I found the tips on managing pain and physical therapy particularly helpful. Can’t wait to start my journey and appreciate the encouragement you’ve provided!
Thank you for sharing such detailed information about knee replacement recovery! The insights on managing pain and the importance of physical therapy were particularly helpful. I’m two weeks post-op and finding your tips on gradual mobility inspiring! Keep up the great work!
Thank you for sharing such detailed insights on knee replacement recovery! I found the timeline of recovery and tips for managing pain really helpful. It’s reassuring to know what to expect in the weeks following the surgery. I’m eager to start my journey and this information has definitely boosted my confidence.
Thank you for sharing such insightful information about the recovery process after a total knee replacement. It’s comforting to know what to expect and how to manage the rehabilitation phase. Your tips on exercises and pain management are particularly helpful. Looking forward to a smoother recovery journey!
Thank you for this informative post! It really helps to know what to expect during recovery after a knee replacement. The tips on managing pain and the timeline for rehab are especially helpful. I’m feeling more prepared for my upcoming surgery!
Thank you for sharing such insightful information about total knee replacement recovery! I found the tips on managing pain and the timeline for returning to daily activities particularly helpful. It’s reassuring to know what to expect and how to prepare for the journey ahead. Looking forward to reading more about your experiences and advice!
Thank you for this informative post! It really helped me understand what to expect during the recovery process after my total knee replacement. The tips on managing pain and the importance of physical therapy are especially useful. I’ll definitely be referring back to this as I prepare for my surgery.
Thank you for sharing such detailed insights on knee replacement recovery! I found the timeline and tips extremely helpful, especially regarding the importance of physical therapy. It’s reassuring to know what to expect during the healing process. Can’t wait to start my own journey!
Thank you for this informative post! It’s great to have a clear understanding of what to expect during recovery after a total knee replacement. The tips about managing pain and staying active are especially helpful. I feel more prepared for my upcoming surgery!
Thank you for sharing such detailed information about knee replacement recovery! It’s reassuring to know what to expect during the healing process. Your tips on physical therapy and managing pain are especially helpful. I’m looking forward to my recovery journey now with a clearer understanding!
Thank you for this informative post! I appreciate the detailed insights on what to expect during the recovery process after knee replacement. It really helps to know the timeline for recovery and the importance of physical therapy. I’m feeling more prepared for my upcoming surgery!
Thank you for this informative post! It’s comforting to know what to expect during the recovery phase after a total knee replacement. The tips on managing pain and staying active are particularly helpful. I’m looking forward to my surgery and appreciate the insight!
Thank you for sharing such detailed insights on the recovery process after a total knee replacement! Your tips on managing pain and setting realistic expectations are incredibly helpful. I’m about to undergo the procedure myself, and I feel more prepared after reading your post. Can’t wait to see the progress after my surgery!
Thank you for sharing such detailed insights on knee replacement recovery! I appreciate the tips on managing pain and the timeline for regaining mobility. It really helps to know what to expect during the healing process. Looking forward to applying these recommendations!
Thank you for sharing such detailed insights on knee replacement recovery! This information is incredibly helpful as I navigate through my own recovery process. I especially appreciated the tips on managing pain and the expected timeline for regaining mobility. It’s reassuring to know I’m not alone in this journey!
Thank you for sharing such detailed insights on the recovery process after total knee replacement. It’s reassuring to know what to expect during rehabilitation, especially regarding pain management and mobility milestones. Your tips on setting realistic goals and the importance of physical therapy will definitely help many of us navigate this journey more smoothly!
Thank you for this detailed guide on knee replacement recovery! I found the timelines and tips really helpful, especially the emphasis on physical therapy. It’s reassuring to know what to expect and how to prepare for the recovery process. Looking forward to my own surgery and following your advice!
Thank you for this informative post! I recently had a total knee replacement, and your insights about the recovery process have been incredibly helpful. It’s reassuring to know what to expect, especially regarding pain management and the timetable for regaining mobility. I appreciate the tips on exercises to start with – those will definitely guide me as I navigate my recovery journey.
This post was incredibly helpful! I appreciated the clear step-by-step outline of what to expect during recovery. I feel more prepared for my upcoming surgery. Thanks for sharing such valuable insights!
Thank you for this insightful post! It really helped to clarify the recovery process after a knee replacement. I appreciate the tips on managing pain and the importance of physical therapy. It’s reassuring to know what to expect during the early stages of recovery.